It's time to evolve
17 years ago, we set out to transform spine surgery.
To disrupt the status quo. To lead and not follow.
And to promote better outcomes to each patient.
The evidence speaks for itself.
More than 400 peer reviewed articles.
And more than 1,000,000 patient lives changed.
Less blood loss,1-7 less time in the hospital1,3-8 and quicker recovery.9-10
This is the new expectation.
More efficient surgery.
While our industry continues to operate “the old way,”
our patients want a better experience.
They deserve a better experience.
It’s time to evolve.
The impact of traditional open approaches
Spine Surgery Evolved
The leader in less invasive surgery
Less invasive surgery is your opportunity to change the way patient care is delivered. The intuitive approach, paired with best-in-class training and a robust procedural portfolio, enables you to confidently adopt less invasive techniques to achieve the same or better outcomes while reducing operative time, blood loss, and length of stay. Our mission hasn’t changed.
XLIF
In 2003, NuVasive revolutionized spine surgery with XLIF, the only lateral approach spine procedure supported by extensive clinical evidence in more than 400 peer-reviewed, XLIF-specific publications. With hundreds of thousands XLIF surgeries since its inception, the procedure continues to transform patients’ lives through reduced blood loss, less time in the OR, and shortened hospital stays as compared to traditional posterior fusion procedures.

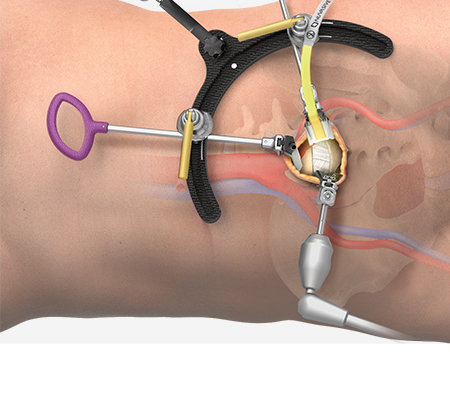
X360
X360 comprises XLIF, XALIF, and XFixation. The integration of these procedures into a single platform allows for the maximum efficiency of using these modern, less invasive techniques while retaining the inherent benefits to surgeons, patients, and hospitals. X360 enables surgeons to treat more patients in the lateral position and further demonstrates our leadership in this space. The system integrates our comprehensive portfolio of biologic, interbody, and fixation offerings, all enabled by Surgical Intelligence.

MAS TLIF
The NuVasive MAS TLIF 2 system offers less invasive, pedicle-based TLIF access and bridges the gap between Open and MIS TLIF approaches. The system features customizable access designed for maximum visibility, functionality, and unimpeded access to known clinical and anatomical landmarks, and integrates with our comprehensive fixation, biologics, and interbody implant portfolio, featuring a wide range of expandable and next-generation static cages.
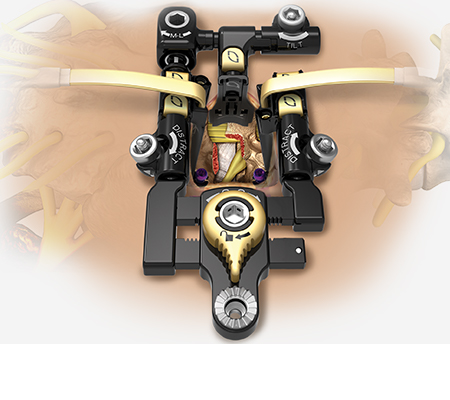
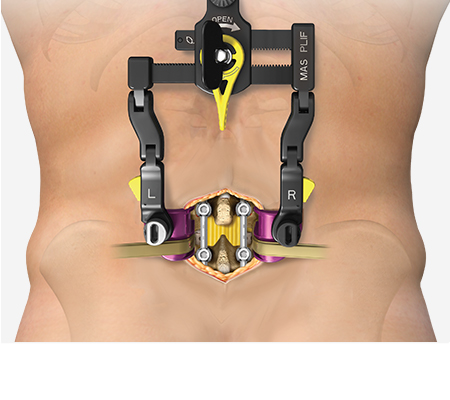
MAS Midline
The NuVasive MAS Midline system provides unimpeded access and direct visualization of anatomy while minimizing unnecessary tissue and muscle disruption through a familiar midline approach. The system features customizable access design to provide patient specific decompression, and integrates with our comprehensive fixation, biologics, and interbody implant portfolio, featuring a wide range of expandable and next-generation static cages.

Procedural integration
Procedural integration
Ready to evolve your practice?
1. Oliveira L, Marchi L, Coutinho E, et al. The use of rh-BMP2 in standalone eXtreme Lateral Interbody Fusion (XLIF®): clinical and radiological results after 24 months follow-up. World Spinal Column J 2010;1(1):19-25.
2. Dakwar E, Cardona RF, Smith DA, et al. Early outcomes and safety of the minimally invasive, lateral retroperitoneal transpsoas approach for adult degenerative scoliosis. Neurosurg Focus 2010;28(3):E8.
3. Goldstein CL, Phillips FM, Rampersaud YR. Comparative effectiveness and economic evaluations of open versus minimally invasive posterior or transforaminal lumbar interbody fusion. Spine 2016;41(8S)S74-89.2.
4. Sembrano, JN, Tohmeh A, Isaacs R, et al. Two-year Comparative Outcomes of MIS Lateral and MIS Transforaminal Interbody Fusion in the Treatment of Degenerative Spondylolisthesis. Spine 2016;41(8S):123-32.
5. Isaacs RE, Sembrano JN, Tomeh AG, et al. Two-Year Comparative Outcomes of MIS Lateral and MIS Transforaminal Interbody Fusion in the Treatment of Degenerative Spondylolisthesis. Spine 2016; 41(8S):133- 44
6. Dhall SS, Wang MY, Mummaneni PV. Clinical and radiographic comparison of mini–open transforaminal lumbar interbody fusion with open transforaminal lumbar interbody fusion in 42 patients with long-term follow-up. J Neurosurg Spine 2008;9:560-5.
7. Whitecloud TS 3rd, Roesch WW, Ricciardi JE. Transforaminal interbody fusion versus anteriorposterior interbody fusion of the lumbar spine: a financial analysis. J Spinal Disord 2001 Apr;14(2):100–3.
8. Lucio JC, VanConia RB, DeLuzio KJ, et al. Economics of less invasive spinal surgery: an analysis of hospital cost differences between open and minimally invasive instrumented spinal fusion procedures during the perioperative period. Risk Manag Healthc Policy 2012;5(5):65-74.
9. Ozgur BM, Agarwal V, Nail E, et al. Two-year clinical and radiographic success of minimally invasive lateral transpsoas approach for the treatment of degenerative lumbar conditions. SAS J 2010;4:41–6.
10. Park Y, Ha JW. Comparison of one-level posterior lumbar interbody fusion performed with a minimally invasive approach or a traditional open approach. Spine 2007;32(5):537-43